WHAT TYPES OF PAIN ARE THERE?
Pain is not one single thing. Different biological mechanisms can contribute to pain, and many people with persistent pain experience more than one type at the same time. That’s why treatment usually works best when it is matched to the main drivers of your symptoms — often combining medical assessment, rehabilitation, education, and practical self-management strategies.
-
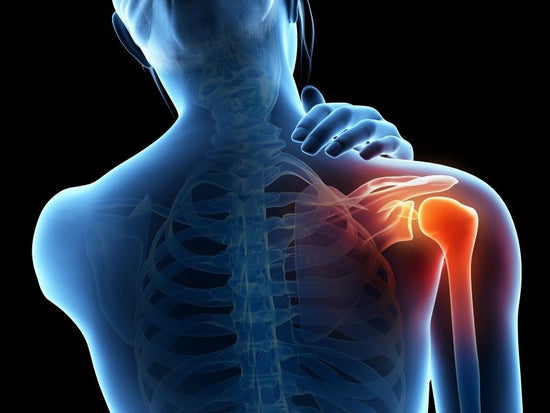
NOCICEPTIVE PAIN
Nociceptors are specialised receptors that respond to actual or potential tissue threat — such as pressure, chemical irritation, temperature extremes, stretch, or reduced blood supply. Nociceptive pain is typically linked to tissue strain or injury and often improves as healing occurs. In persistent pain, nociceptive input can still play a role when joints, muscles, or other structures remain irritated or inflamed.
-
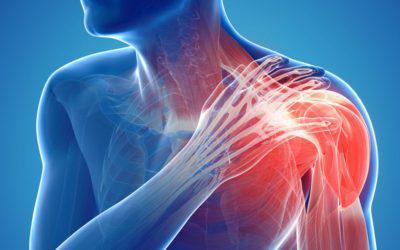
NEUROPATHIC PAIN
Neuropathic pain occurs when a nerve (or the spinal cord/brain) is affected by damage or disease. It is often described as burning, shooting, electric, or tingling, and may be associated with numbness or altered sensation. Neuropathic pain does not always respond well to simple painkillers and often needs targeted medication, rehabilitation, and treatment of the underlying cause where possible.
-
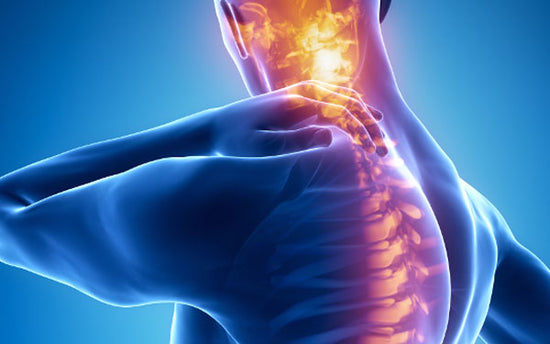
NOCIPLASTIC PAIN
Nociplastic pain refers to pain arising from changes in how the nervous system processes and amplifies danger signals. The system becomes over-protective and produces pain even without ongoing tissue damage. This is common in long-standing pain conditions and is often improved through education, graded activity, sleep and stress regulation, and rehabilitation strategies that retrain the system over time.
FACTS ABOUT CHRONIC PAIN
Persistent pain can be confusing and exhausting — and knowledge helps you make better decisions. These key facts explain why pain can behave in unexpected ways, and why comprehensive assessment and a multi-dimensional plan are often more effective than a single “magic” treatment.

FACT 1:
The intensity of pain is not always directly related to how much tissue damage is present. In persistent pain, flare-ups can occur even when scans look unchanged, because factors like inflammation, stress, poor sleep, and sensitisation can increase pain sensitivity. If your pain is new, worsening, follows significant injury, or is associated with red-flag symptoms (weakness, numbness, bladder/bowel change, fever, unexplained weight loss), seek assessment promptly.

FACT 2:
Pain is not always felt where the source of the problem is. Some pain is “referred,” meaning it is experienced in one place even though the contributing structures are elsewhere. This happens because nerve signals can converge in shared pathways. For example, irritation in the neck can be felt in the shoulder, arm, or hand. Proper assessment helps clarify what is driving symptoms and which treatments are appropriate.

FACT 3:
Pain can be real even when the tissue is not being damaged. Nerves can become irritated or sensitised, producing pins and needles, burning, or shooting pain even without injury at the area where symptoms are felt. This does not mean the pain is imaginary — it means the nervous system is amplifying warning signals. A clinical assessment can help determine whether symptoms reflect temporary irritation or something that needs urgent attention.

FACT 4:
You do not always need an injury to develop persistent pain. Sometimes there is an identifiable underlying condition (such as arthritis, inflammation, or nerve compression). In other cases, routine tests do not show a single clear structural cause, and the nervous system itself may become sensitised over time. Either way, the goal is to identify likely contributors and build a plan that improves function, reduces flare-ups, and supports long-term health.
TREATMENT OPTIONS - A COMBINATION APPROACH
-
TREATING PAIN WITH MEDICATION
Medication may be used to reduce pain and improve your ability to participate in other parts of your treatment plan, such as movement, rehabilitation, sleep, and lifestyle changes. Different medicines are used for different pain mechanisms and may include anti-inflammatory medicines, analgesics (pain relievers), and adjuvant medications that target nerve or pain-processing pathways. Your clinician should explain what the medication is for, how to take it safely, how long it is intended to be used, and what side effects or risks to watch for — and you should discuss any concerns or unexpected effects promptly.
-

THERAPY APPROACHES
Chronic pain is often best managed with an interdisciplinary rehabilitation approach that addresses function, movement, daily activity participation, and lifestyle contributors — not symptoms alone. At PAIN, rehabilitation may involve physiotherapy, occupational therapy, biokinetics, and dietetics, depending on your needs. These non-pharmacological interventions can support nociceptive, neuropathic, and nociplastic pain by improving strength, capacity, confidence in movement, pacing strategies, and overall health. When tailored and coordinated, rehabilitation becomes a key part of long-term self-management and better quality of life.
-

WHEN AND WHY DO I NEED A PAIN PROCEDURE?
Pain procedures may be helpful for nociceptive pain and selected components of neuropathic pain, particularly when symptoms are linked to conditions such as osteoarthritis or inflammatory joint disease and conservative measures are not enough. These procedures do not treat the underlying condition itself; they aim to reduce pain so that you can participate more effectively in rehabilitation, movement, and self-management strategies. They are generally not effective for nociplastic pain, but in mixed pain presentations, reducing the nociceptive “volume” may create space to address sensitisation through other treatments. Effects are temporary and vary between individuals; some radiofrequency-based techniques can provide relief for months and, in selected cases, longer. Outcomes are best when procedures are part of a broader, individualised plan.
-

SURGERY
Surgery may be considered when there is a clear structural problem, progressive neurological compromise, spinal instability, or when appropriate conservative treatment has not achieved adequate control of symptoms. The decision is based on your history, examination, imaging, overall health, and functional goals — and includes a careful discussion of benefits, limitations, risks, and realistic recovery expectations. In many cases, surgery aims to address a specific anatomical issue (such as nerve compression or instability) rather than “cure” all pain. Rehabilitation and lifestyle strategies are often still important after surgery to optimise long-term outcomes. If surgical assessment is appropriate, your team can guide you and arrange referral to a suitably qualified specialist.
WHEN DO I NEED SURGERY?
Only a minority of people attending chronic pain clinics ultimately need surgery. Many patients we see have already had surgery elsewhere and still experience pain, which often reflects that persistent pain can be driven by multiple mechanisms — including inflammation, joint degeneration, nerve sensitivity, and central sensitisation. Understanding when surgery is helpful, and when other approaches are more appropriate, is an important part of making informed decisions.
MYTH 1: SURGERY CAN CURE BACK OR NECK PAIN
Surgery can be essential for certain conditions, but it does not “cure” every cause of chronic back or neck pain. For example, osteoarthritis of spinal joints is common and may contribute significantly to pain, and surgery cannot reverse arthritis itself. In selected cases, surgery can improve stability or relieve nerve compression, but long-term outcomes depend on the underlying diagnosis, careful patient selection, and ongoing rehabilitation and self-management.
MYTH 2: IT IS MY BULGING DISC THAT IS CAUSING MY PAIN
Disc bulges are common and can be seen on scans even in people without pain. Imaging findings must be interpreted alongside symptoms and examination. Pain may come from discs, joints, muscles, nerves, inflammation, or sensitisation — and the purpose of assessment is to identify the most likely contributors in your case, not to treat a scan result in isolation.

MYTH 3: PINS AND NEEDLES IN MY ARMS OR LEGS MEANS THAT I AM DAMAGING A NERVE
Pins and needles can have many causes, ranging from temporary irritation to problems that need urgent assessment. If symptoms are new, worsening, persistent, or associated with weakness, balance changes, or bladder/bowel symptoms, seek medical attention promptly. In many cases, pins and needles reflect irritation or inflammation rather than permanent damage — but it is important to assess the pattern properly.

MYTH 4: I WILL BE PARALYSED IF I DO NOT HAVE AN OPERATION
Severe neurological deterioration is uncommon, but it must be taken seriously. If you develop progressive weakness, difficulty walking, loss of coordination, or changes in bladder or bowel control, seek urgent assessment. Many episodes of radiating pain improve with conservative care, and surgery is only required in a small subset of cases — the key is recognising when urgent evaluation is needed.

MYTH 5: MY DOCTOR TESTED FOR ARTHRITIS, AND I HAVE NONE
“Arthritis” includes many conditions. Some inflammatory arthritides can be supported by blood tests, but osteoarthritis cannot be diagnosed on a blood test. Imaging can assist, but results must be interpreted clinically and none are perfect. Your clinician will use history, examination, and appropriate investigations to determine whether arthritis is contributing to your pain and what type of management is most appropriate.
THERE ARE 3 MAIN SPINAL SURGERY INDICATIONS
Spinal surgery is generally considered in a small number of scenarios, including: (1) serious neurological compromise where delaying treatment may be unsafe, (2) tumours affecting the nervous system that require surgical management, and (3) fractures or instability that are unlikely to heal adequately without intervention. These situations are typically guided by clear clinical findings and imaging, and often require urgent or specialist assessment.
TYPES OF SPINAL SURGERY
Spinal surgery is broadly performed for two reasons: to relieve pressure on nerves (decompression) or to stabilise the spine (fixation/fusion). Techniques range from smaller, targeted procedures to more complex reconstructions, and may be performed through open, minimally invasive, or endoscopic approaches depending on the condition and goals of surgery. Your surgeon will recommend the least invasive option that is appropriate for your specific diagnosis and risk profile.
TREATING THE DISEASE
When persistent pain is linked to long-term conditions, the most meaningful improvements often come from improving the health of the whole system — reducing inflammation where possible, restoring movement capacity, improving sleep, regulating stress, and building sustainable routines. Medical care supports this process, but the most durable results usually come from consistent day-to-day actions that fit your life and are guided by an experienced team.
-

DIETS AND MEALS TO COMBAT PAIN
Dietitians support pain care by helping patients make practical, evidence-based nutrition choices that improve overall health and may reduce inflammation risk factors. Nutrition support can be especially helpful for weight management, metabolic health, gut symptoms, and energy levels — all of which can influence pain, recovery, and function. The aim is not perfection; it is a sustainable eating pattern that supports your condition and goals.
-

MOVEMENT IS MEDICINE
Persistent pain often leads to less movement, which can reduce strength and confidence and make pain more sensitive over time. Graded movement and exercise, introduced at the right level and progressed safely, can help restore capacity and reduce flare-ups. A rehabilitation team can help you pace activity, avoid boom-and-bust cycles, and build a plan that is realistic and safe for your diagnosis.
-

THERAPY FOR PAIN
Pain rehabilitation is about improving function, independence, and quality of life — not just treating symptoms. Therapists help you build strategies for daily activities, confidence in movement, pacing, and long-term self-management. These skills remain useful beyond the current flare-up and form a foundation for durable improvement.
OTHER TERMINOLOGY YOU MIGHT HEAR
Referred Pain
Referred pain is felt in one area even though the contributing structures are elsewhere. It is often deep, can follow patterns linked to specific nerves, and commonly occurs because multiple tissues share nerve pathways to the spinal cord and brain. Assessment helps identify likely sources and guide the right treatment.
Peripheral Sensitisation
Peripheral sensitisation is a normal part of healing. When tissues are irritated or inflamed, nearby nerves become more responsive and send stronger warning signals to the brain. This increased sensitivity can make normal movement or touch feel more painful for a period, even when damage is not worsening.
Central sensitisation
Central sensitisation refers to increased sensitivity within the brain and spinal cord after pain has persisted for a long time. The nervous system becomes over-protective, producing stronger pain responses to normal inputs such as movement, stress, or poor sleep. The good news is that sensitisation can often improve over time with education, graded activity, rehabilitation, and supportive lifestyle strategies.
Endogenous Opioids
Your body produces its own pain-relieving chemicals (endogenous opioids), especially with regular movement, supportive sleep, and positive social connection. This is one reason carefully paced exercise can help persistent pain over time — it supports natural pain modulation rather than relying only on external pain relief strategies.
Sensitivity to physical activity
When the nervous system is sensitised, exercise can initially flare pain, which can feel confusing and discouraging. This does not necessarily mean damage is occurring — it often means the system is over-reactive. The goal is to find the right starting point and build capacity gradually, so movement becomes safer and more tolerable over time. A graded plan guided by your team helps you progress without triggering repeated flare-ups.












